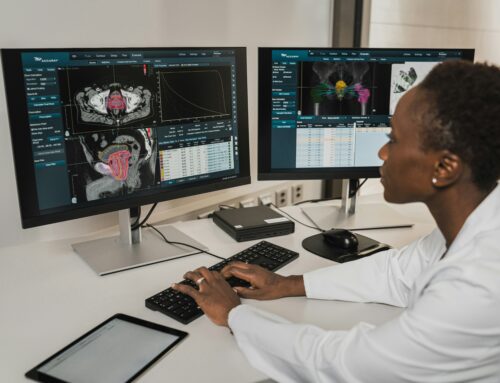
Why are appetite, nutrition and weight relevant to cancer survivors?
Cancer leads to several metabolic alterations, such as inflammation and increase of body energy expenditure. Frequently, appetite is suppressed, which leads to a reduction in food intake. Thus, despite more energy being used by the body, less energy is introduced. This results in weight and muscle mass loss, as well as muscle strength impairment. Furthermore, nutritional deficiencies and fatigue may also occur.
Beyond cancer-related malnutrition, also cancer treatments may contribute to malnutrition through treatments’ side-effects, such as loss of appetite, fatigue, bowel distress, impairment or absence of taste, olfactory changes, nausea, and mouth sores, among others [1]. After treatment, some of these symptoms may remain, and therefore impact the quality of life of cancer survivors.
Furthermore, many cancer survivors are at increased risk for weight gain either during or after treatment. For example, over 50% of breast cancer survivors in Western countries have obesity or are overweight. Considering that obesity is associated with increased risk of developing cancer, maintaining an adequate body mass index and body composition is thus a priority in cancer survivors [2]. Indeed, leading cancer organizations recommend that cancer survivors achieve and maintain a healthy body weight, with modest weight loss (5 to 10% of body weight) recommended for those with excessive weight [2]. Ultimately, weight management through diet and exercise can help prevent recurrence, additional primary cancers, and other chronic diseases.
How can we improve nutrition in cancer survivors?
Informed lifestyle choices are thus crucial to improve long-term outcomes of cancer patients. However, improving dietary patterns is challenging for cancer survivors. This is due to several factors, spanning from secondary disabilities and the effects of treatment, to altered metabolism. Furthermore, when cancer survivors research diet options, they frequently encounter ambiguity and an abundance of misinformation. Therefore, a personalized dietary approach, aiming to achieve individual needs of macro and micronutrients, should be considered for these patients.
What can we learn from appetite and feeding behavior-related research?
The Neuropsychiatry Unit at the Champalimaud Research & Clinical Centre is focused on researching reward-related feeding behavior, ranging from experiments that explore normal physiology in rodent models [3], to research on dysfunctional feeding behavior in patients with obesity [4]. We have been particularly interested in how the reward from feeding is associated with obesity, which was shown at a population level using the Power of Food Scale [4]. Furthermore, we recently published results of a multicenter longitudinal cohort, including more than 200 bariatric patients, showing weight-loss prediction according to the same measure, as well as by a gustatory measure of sweet taste intensity, with patients with higher sweet intensity ratings before surgery losing more weight [5].
In fact, altered taste perception has long been associated with several diseases, including obesity [6], as well as cancer and cancer treatments. For example, radiation-induced taste dysfunction negatively affects the nutritional status of patients and their quality of life [7], and may remain months or even years after treatment. There is urgent need for further research on the impact of cancer and cancer treatments on taste, and the relationship with weight trajectories in cancer survivors.
How can better nutrition benefit cancer survivors?
As highlighted throughout this article, nutrition is a determinant factor in cancer management. The detrimental effects of the disease and related treatments on dietary intake and body composition have been shown to impair the quality of life of the patients and have been associated with reduced survival rates [8].
Cancer survivors, when compared to individuals without a history of cancer, had poorer nutritional intake [9]. This was shown particularly with regard to higher consumption of ‘empty calories’ (e.g., solid fats, alcohol, and added sugars) and lower dietary intakes of fiber, vitamin D, vitamin E, potassium, and calcium [9]. Providing individualized nutritional advice can improve dietary intake and potentially prevent weight loss or weight gain, as well as vitamin and mineral deficiencies.
Are there any tips for weight management after cancer?
Cancer survivors experiencing appetite loss, who are at risk of becoming underweight, should consume smaller and more frequent meals. They should also consume minimal liquids during meals in order to increase food intake, and consume them in between meals instead to avoid dehydration. In addition, for those who cannot meet their nutritional needs through foods alone, fortified, commercially prepared, or homemade nutrient-dense beverages or foods can improve the intake of energy and nutrients [10].
Furthermore, it is well recognized that muscle mass maintenance is crucial since reduced muscle mass as a result of cancer-induced cachexia is associated with fatigue and impaired physical function [8]. However, in some patients, for example those with excess weight, muscle wasting is not evident. Thus, body composition monitoring is a simple but important behavior that all cancer survivors can adopt.
These findings reinforce the need for dietary interventions in cancer survivors. Oncology care providers play an important role in reinforcing the importance of an adequate dietary intake, and can refer patients to registered dietitians who are experts in oncology care or to other reputable sources [10], such as the European Cancer Patient Coalition, in order to improve the overall quality of life of cancer survivors.
Authors: Marta Carriço1 and Gabriela Ribeiro, MSc2,3.
1 Registered dietitian-nutritionist. Champalimaud Clinical Centre, Lisbon, Portugal.
2 Registered dietitian-nutritionist. Champalimaud Research & Clinical Centre, Lisbon, Portugal.
3 Lisbon Academic Medical Centre PhD Programme. School of Medicine, University of Lisbon, Lisbon, Portugal.
References
- Arends J, Baracos V, Bertz H, et al. ESPEN expert group recommendations for action against cancer-related malnutrition. Clin Nutr. 2017;36(5):1187-1196. doi: 10.1016/j.clnu.2017.06.017.
- Reeves MM, Terranova CO, Eakin EG, Demark-Wahnefried W. Weight loss intervention trials in women with breast cancer: a systematic review. Obes Rev. 2014;15(9):749-768. doi:10.1111/obr.12190.
- Fernandes AB, Alves da Silva J, Almeida J, et al. Postingestive Modulation of Food Seeking Depends on Vagus-Mediated Dopamine Neuron Activity. Neuron. 2020;106(5):778-788.e6. doi:10.1016/j.neuron.2020.03.009.
- Ribeiro G, Camacho M, Fernandes AB, Cotovio G, Torres S, Oliveira-Maia AJ. Reward-related gustatory and psychometric predictors of weight loss following bariatric surgery: a multicenter cohort study [published online ahead of print, 2021 Feb 9]. Am J Clin Nutr. 2021;nqaa349. doi:10.1093/ajcn/nqaa349.
- Ribeiro G*, Camacho M*, Santos O, Pontes C, Torres S, Oliveira-Maia AJ. Association between hedonic hunger and body-mass index versus obesity status. Sci Rep. 2018;8(1):5857. Published 2018 Apr 11. doi:10.1038/s41598-018-23988-x.
- Ribeiro G, Oliveira-Maia AJ. Sweet taste and Obesity. [published online ahead of print, 2021 Feb 13]. Eur. J. Intern. Med. doi:https://doi.org/10.1016/j.ejim.2021.01.023.
- Gunn L, Gilbert J, Nenclares P, Soliman H, Newbold K, Bhide S, Wong KH, Harrington K, Nutting C. Taste dysfunction following radiotherapy to the head and neck: A systematic review. Radiother Oncol. 2021 Feb 3; 157:130-140. doi: 10.1016/j.radonc.2021.01.021.
- Ryan A.M., Power D.G., Daly L., Cushen S.J., Bhuachalla Ē.N., Prado C.M. Cancer-associated malnutrition, cachexia and sarcopenia: The skeleton in the hospital closet 40 years later. Nutr. Soc. 2016;75:199–211. doi:https://doi.org/10.1017/S002966511500419X
- Zhang F.F., Liu S., John E.M., Must A., Demark-Wahnefried W. Diet quality of cancer survivors and noncancer individuals: Results from a national survey. 2015;121:4212–4221. doi:https://doi.org/10.1002/cncr.29488
- Rock CL, Doyle C, Demark-Wahnefried W, Meyerhardt J, Courneya KS, Schwartz AL, Bandera EV, Hamilton KK, Grant B, McCullough M, Byers T, Gansler T. Nutrition and physical activity guidelines for cancer survivors. CA Cancer J Clin. 2012 Jul-Aug;62(4):243-74. doi: 10.3322/caac.21142.