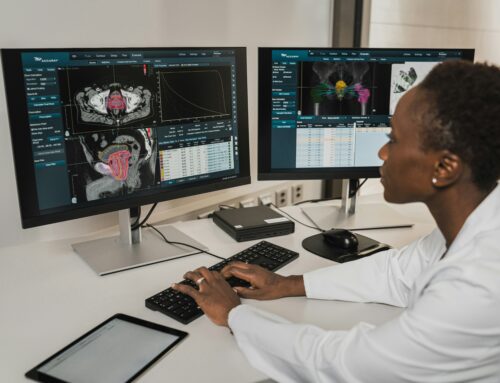
The healthcare sector is currently experiencing a transformative boom, driven by the adoption of innovative technologies. Robotics, Artificial Intelligence, Internet of Things, 4G and 5G mobile communication, blockchain, and supercomputing are just a few examples. Digital transformation is creating opportunities to re-shape how we receive and provide health and care services in a digital Europe. Technologies are changing the way we gather, process, control and use data, as well as enabling an organizational change. Ultimately, this benefits people, empowering patients, health care systems, and the economy.
The FAITH project aims to be part of it by developing and piloting a federated machine learning-based solution for improving diagnosis of depression and anxiety in cancer survivors. Nearly half of the women diagnosed with breast cancer report clinically significant emotional or psychological distress after treatment. Quite often, such psychological changes go unnoticed, or are dismissed, and therefore are neglected. Untreated symptoms of depression and anxiety may hinder quality of life of women that are survivors of breast cancer. On the other hand, quality of life is being studied as a determinant parameter in the treatment of cancer patients, confirming its relevance to them.
Depression and anxiety in breast cancer survivors
Once chemo and/or antitumoral treatment is over, breast cancer survivors may develop feelings of sadness and fear, issues with their body image, and even depression and anxiety. Such feelings depend on different factors and on a patient’s social and emotional profile as cancer survivor. Even if breast cancer survivors continue with Hormone Therapy (HT), the anxiety or insecurity feelings could appear. Cancer survivors might also express fear of recurrence and feelings of loss of support from family, friends, and the health team that have attended them. The latter, in particular, may be conditioned by the loss of regular contact with their doctor.
Emotional distress may increase until the next medical control appointment. Often, these spread out over time, causing a perception of prolonged uncertainty about cancer prognosis. Emotional stressors can occur depending on a patient’s health and wellbeing level as well as on many other factors. For example, employment status, relationship with family or friends, alterations in body image, a decrease in the level of functional autonomy, or changes in the roles resulting from the physical consequences of treatment may affect the emotional status of a patient.
Ultimately, these is a risk of misclassifying symptoms of emotional distress as cancer-related symptoms, or vice-versa. Symptoms that are present after completing a primary cancer treatment can persist for more than 5 years. As a result, they can significantly reduce survivors’ quality of life and functional outcomes, including work productivity. A comprehensive evaluation is then crucial, especially when such symptoms present too often, for too long.
Artificial Intelligence: supporting breast cancer patients
The Universidad Politécnica de Madrid, Hospital Gregorio Marañón and FAITH project partners seek to maximize the potential of Federated Learning techniques to support breast cancer survivors. But what is Federated Learning, exactly? Federated Learning is a Machine Learning method that trains an algorithm through multiple decentralized devices or servers containing local data samples, without exchanging them with third parties. Thus, it preserves the patients’ privacy by design (see Google’s Federated Learning comic).
Nowadays, many healthcare organizations are exploiting this paradigm. For example, companies like NVIDIA are trying to improve breast cancer diagnosis through their CLARA Federated Learning software.
Recently, an international group of hospitals and medical imaging centres evaluated AI models for the interpretation of mammography formed with federated learning techniques. The study demonstrated that these techniques outperformed neural networks formed with data from a single institution, without compromising patients’ privacy.
Finally, the use of Machine Learning methods may help to give insights on patients’ satisfaction with the outcome of an intervention when using patient centric approaches.
FAITH will develop models based on Federate Learning techniques able to detect negative trends in mood and quality of life. We will use the latest advances of applying Machine Learning for detecting depression and for assessing quality of life. We will also provide a FAITH mobile app as an important tool to dispense psychosocial care to breast cancer survivors. By focusing on issues of their interest, and evaluating their experience based on the value of care they receive, FAITH will be an empowering tool for cancer patients, in the end.
Piloting an AI-based solution to support breast cancer survivors
Madrid region, through Hospital Gregorio Marañón (SERMAS) and Universidad Politécnica de Madrid (UPM), will be a pilot for FAITH technologies. It will use the FAITH app and Federated Machine Learning techniques for a non-intrusive monitoring of cancer patients’ lifestyle.
The pilot will rely on wearable sensors and the patients’ mobile phone to monitor several health indicators in cancer survivors. These indicators comprise, for example, physical activity, quality of sleep, outlook, appetite, and social activity. FAITH will use a Federated Machine Learning approach to enable a continuous monitoring and processing of these objective data. This will guide a personalized patient support, not only for lifestyle goals but also for data-driven coaching. The ultimate aim is getting to a better model for mental health monitoring for improving breast cancer survivors’ rates for depression, anxiety, and quality of life during the follow-up period.
The potential of gathering this behavioural information from patients will overstep the FAITH project. In the end, it will enrich new models that shall support health providers’ decision making for improving the diagnosis of depression and anxiety, reducing their symptoms, as well as improving the health and well-being of cancer survivors.
Authors:
Ma. Eugenia (Xenia) Beltran, Javier Rojo, Cecilia Vera, and Samantha Villanueva of the Universidad Politécnica de Madrid (UPM).
Miguel Martín, María del Monte Millán, Tatiana Massarrah, and Sara López-Tarruella of the Hospital Gregorio Marañón (SERMAS).